How is Behçet’s pronounced?

Behçet’s is usually pronounced as “Beh-CHETS” after Hulusi Behçet a Turkish Professor of Dermatology, who spent many years promoting the clinical awareness of the condition.
Is Behçet’s syndrome’ the same as
Behçet’s disease’?
Whilst this condition has been given many names over the years, the two most widely accepted are Behçet’s syndrome and Behçet’s disease. We favour using “syndrome” over “disease”, because syndrome correctly suggests that not every patient has exactly the same condition, whilst disease implies a single entity. There is also no specific test for making the diagnosis.
What is Behçet’s Syndrome?
Behçet’s syndrome is an inflammatory condition that may affect almost any part of the body. Often the skin and the lining of the mouth and genital areas (mucosa) can be inflamed, causing ulcers or rashes. Joint pains, headaches, tiredness and stomach pains are also common. In some people, the eyes, blood vessels or (rarely) the brain or nerves may become involved.
Who are affected?
Behçet’s syndrome is most common along the ancient silk trading routes stretching from the Far East to the Mediterranean, and appears to have the highest frequency in Turkey and surrounding regions.
It is very rare in the UK and other Northern European countries and may occur in people of any nationality and race. Men and women are probably affected with equal frequency, but it is sometimes more severe in men. It may occur at any age, but is diagnosed most commonly in adults in their 20s and 30s and, whilst it can occur in young children, this is unusual.
What is the aetiology (cause)?
Genetics
Behçet’s syndrome is not well understood by medical professionals. Genetic studies suggest that the gene HLA B-51, which plays a role in immunity, is present more often in people affected by this disease. Having an affected family member very slightly increases the risk of developing the condition. As the syndrome is not present from birth, doctors feel that it is likely that genes aren’t the only factor involved. Indeed, if one of a pair of identical twins (who have identical genes) develops Behçet’s Syndrome, the other twin will not necessarily develop the condition.
Environmental Triggers
Since genetics alone cannot explain the development of this condition, it is likely that an environment factor(s) trigger is required to cause Behçet’s syndrome to develop in individuals with a genetic predisposition. Researchers have studied many possible triggers ranging from viruses (e.g. Herpes cold sore virus), bacterial infections (e.g. bacteria that cause a ‘Strep throat’), smoking, and the bacteria that live in the bowel, but so far have not been able to identify the underlying trigger.
Resultant abnormal inflammation
The result of the interaction between genes and an as yet unknown environmental factor is that someone develops abnormal inflammation, which causes the features of Behçet’s Syndrome. In the right situation, such as as in the fight against infection, inflammation plays a crucial role in health. However, the inflammatory response appears to be too enthusiastic in people with Behçet’s syndrome an even small insults to the body (e.g. a thorn prick) may result in a big inflammatory response, and inflammation may also occur without an obvious cause.
What are the symptoms?
Ulcers
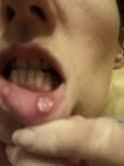
Recurrent mouth ulcers are the hallmark of Behçet’s syndrome. Almost all patients have experienced these, and they can predate other symptoms by months or even years. Ulcers can be small, large or multiple. They are often on the inner lips but can also occur on the tongue, the roof of the mouth and occasionally in the throat. Ulcers in Behçet’s syndrome do not typically form on the external lips. The ulcers are usually painful and occasionally leave a scar. Mouth ulcers affect up to 10% of otherwise healthy people, so having mouth ulcers alone is not enough for a diagnosis of Behçet’s Syndrome. Importantly, many other medical conditions can also be associated with mouth ulcers. Most oral ulcers in Behçet’s syndrome resolve within 10-14 days, although replacement with new ulcers may make it feel as if they are sustained. If an ulcer is persistent, your doctor may wish to arrange a biopsy to look into the diagnosis.
Genital ulcers occur less frequently than oral ulcers. In Europe approximately 60-70 per cent of people with Behçet’s Syndrome report suffering from them. They resemble mouth ulcers in appearance, are usually painful and, when deep, may heal with scarring. Genital ulcers in females affect the vulva and vagina and occasionally the cervix. In males, ulcers occur typically on the scrotum. Because of their location, genital ulcers may become infected. They can be triggered by sexual intercourse and, conversely, are an obvious impediment to sex. As with oral lesions, non-healing ulcers should be biopsied.
Skin
Skin problems are very common in Behçet’s syndrome, occurring in about 80 per cent of patients. Usually people will report redness and spots (pustules) resembling acne. Steroid treatment may also cause acne, which can make it hard to establish if the pustules are related to the Behçet’s Syndrome or are rather a side effect of treatment.
Less commonly, tender lumps may develop on the shins that resemble bruises (erythema nodosum), or which are due to an inflamed vein under the skin.
Pathergy
“Pathergy” is a term that describes an inappropriately large response to minor trauma. It is often experienced as prolonged or severe redness and local swelling at the site of a day-to-day injury, such as a needle or thorn prick, or a nettle sting. The “Pathergy test” involves using a sterile hypodermic needle to make a deep prick in the forearm skin of the patient. A positive test is where a small swelling (papule), possibly with pus (pustule), develops at the site of the needle prick 24-48 hours later. If positive, the test is useful. However, a significant proportion of patients with Behçet’s Syndrome will have a negative test and some other conditions are also associated with pathergy.
Eyes
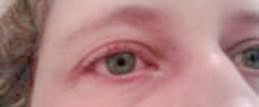
Eye inflammation may be a serious problem in some people with Behçet’s Syndrome. It is thought that 50-70 per cent of people with Behçet’s develop inflammation of the eye. If this is going to happen, it usually starts within 2-3 years of the diagnosis of Behçet’s syndrome. It is the first symptom (or the one that leads to the diagnosis) in 10-15 per cent of cases. Eye inflammation usually comes on in unpredictable, repetitive attacks. Specialist help should be sought quickly if any symptoms develop, as prompt treatment is required to avoid damage to sight.
Headache
Headaches are very commonly reported in people with Behçet’s syndrome. Over 80 per cent of people will report this symptom. For the vast majority, headaches are not the result of a serious problem in the brain and typically improve with symptomatic treatment.
Symptoms that warrant further investigation include very severe or incapacitating pain, a change in character of the headache and particularly the presence of other symptoms (e.g. weakness, speech difficulties, visual loss). Serious brain problems occur in only a small proportion of patients with Behçet’s syndrome.
Muscle and joint pains
Pain in the muscles and joints are frequently found in Behçet’s syndrome. Occasionally joint swelling and tenderness (arthritis) occurs, but this is rarely persistent. Even if arthritis does occur, it rarely leads to damage to the joints and seldom becomes a significant cause of disability.
Stomach pains
Many patients with Behçet’s syndrome experience abdominal pains, and symptoms similar to “irritable bowel syndrome” (bloating, diarrhoea or constipation). Camera tests such as colonoscopy / OGDs are frequently normal despite symptoms, with only about 1 in 10 symptomatic patients having visible ulceration or inflammation on these tests. Symptoms may respond to irritable bowel syndrome treatments or, when ulcers are present, by treatment with immunosuppressive drugs.
Blood clots and blood vessels
Less than 1 in 10 European patients with Behçet’s syndrome develop inflammation in blood vessels. The blood vessels most often affected are veins. Veins of any size or position may be involved, but particularly the deep veins of the legs, causing Deep Vein Thrombosis (DVT). Arteries are less commonly affected. Aneurysms (expansion of arteries) can occasionally occur.
There is no good evidence that Behçet’s syndrome predisposes to ordinary heart disease.
Tiredness
Most patients with Behçet’s syndrome report feeling fatigued and this may well impact on quality of life. The reasons for fatigue are often complex, often including inflammation, loss of physical fitness, pain, low mood and/or poor sleep. In addition to treatments to suppress the inflammation, attempts to increase fitness (e.g. swimming or pilates), address sleep disturbances, pain and mood may improve this symptom.
Making a diagnosis
No diagnostic laboratory or imaging test currently exists for Behçet’s syndrome.
A doctor will probably wish to undertake blood tests to help out rule other types of illness and to record the amount of inflammation. However, “inflammatory marker” blood tests (eg ESR, CRP) may be normal or only modestly raised despite ongoing clinical symptoms.
One blood test that may be helpful is “HLA-B51 expression”. HLA B51 is a protein that is found on the surface of blood cells. People differ in the exact HLA proteins on the surface of their cells, and ‘HLA B51’ is the one found quite frequently found in people with Behçet’s Syndrome. It is important to realise that many people with Behçet’s syndrome will not have this protein, and, equally well, most people who have this protein will never develop Behçet’s Syndrome.
The diagnosis therefore has to be decided on clinical grounds (i.e. on the basis of the opinion that your doctor forms after talking to you, examining you, and after taking blood tests to rule out other illnesses).
Clinical classification criteria
There are many different clinical classification criteria developed to help classify Behçet’s Syndrome. The fast that thee are so many indicates how difficult this can be. Perhaps the most widely used are those developed by a group of doctors in 1990 for standardising patients for research studies. It is possible to still have Behçet’s syndrome without fully fulfilling these research criteria.
The Classification criteria published by the International Study Group in 1990
- Oral ulcerations occurring at least three times a year
- Plus two of the following in the absence of other systemic diseases:
- recurrent genital ulcers
- specific eye lesions observed by an ophthalmologist
- skin lesions consistent with Behçet’s syndrome
Treatment
The general approach to treatment is to tailor therapy to the organ involved and severity of involvement. Some patients just require short term treatment to cover a flare. Others may require immunosuppressive treatment with biologic drugs to prevent and minimise disease activity. The three UK Centres of Excellence for Behçet’s syndrome have developed a national drugs pathway to help doctors choose treatment: http://www.behcets.nhs.uk
Ulcers
The aim of therapy is to reduce the frequency and severity of ulcers to an acceptable level. Topical measures should be tried first when possible, particularly in mild disease. Focusing on oral hygiene by using chlorhexidine mouth washes to reduce bacterial growth may reduce the frequency of mouth ulcers and subsequent infection. Topical corticosteroids are often helpful, as suggested by their widespread use rather than by robust clinical trials. These agents can be applied in many ways, including a beclomethasone inhaler (designed for asthma) to spray onto incipient lesions as they first become symptomatic, triamcinolone acetonide in adhesive bases or hydrocortisone lozenges.
Local steroid preparations may also be applied to genital ulcers, using an inhaler spray or cotton tips. Sucralfate can be used as an oral rinse or directly applied to genital ulcers.
Colchicine is usually the first-line tablet therapy for orogenital ulceration when topical measures are inadequate. Many patients will require further escalation in therapy and azathioprine is the usual first choice. If this therapy fails, an alternative can be chosen from the list below with due consideration of toxicity and cost.
Skin disease
Skin rashes may require treatment by steroids, which can be given as a cream or ointment (such as betnovate), as tablets (prednisolone) or intra muscular injection (depomedrone). Colchicine may be often helpful and azathioprine sometimes used. When these medicines are not tolerated or don’t work, biologic drugs such as infliximab or interferon are used.
Eye disease
Eye involvement in Behçet’s syndrome must be treated promptly, and with supervision by an ophthalmologist. The aim is to stop inflammation in the eye and prevent loss of sight. This can be achieved through steroid eye drops, injections, administration of immunosupressants such as azathioprine, or biologic drugs such as infliximab or interferon.
Other organ involvement
The same principles are used to treat Behçet’s symptoms in other organs. Headaches can often respond to anti-migraine treatments and joint pains to anti-inflammatory drugs. Again, where the disease is flaring badly and inflammation id not controlled, immunosuppressive or biologic drugs may be required. In England, funding for biologic drugs is help by the three Centres of Excellence.
Drugs and Side effects
For information on the main drugs prescribed for Behçet’s Syndrome see:
- Colchicine
- Azathioprine
- Methotrexate
- Steroids
- Cyclophosphamide (for severe illness)
- Infliximab
- Adalimumab
- Etanercept
- Interferon alpha (Roferon)
Whilst thalidomide has been used for Behçet’s syndrome in the past, it is now only very rarely used as other drugs are both more effective and are safer.
For information on other drugs used in the treatment of vasculitis see Glossary of drugs and side effects.
General considerations
Lifestyle modifications to reduce stress should be considered as many people report that stress exacerbates Behçet’s syndrome. It is often worthwhile checking for and correcting vitamin D deficiency, as vitamin D has many immune-modulating effects and is often at surprisingly low levels in people from Northern Europe.
Surgery and Behçet’s Syndrome – what should I know?
Given the large inflammatory response that people with Behçet’s syndrome mount to trauma, surgery should not be undertaken lightly. A course of steroids, such as prednisolone, starting a few days preoperatively and reducing rapidly after the procedure may be helpful. This should be discussed with your specialist and surgeon, as it may help prevent inflammatory complications developing around the time of the operation. However, the risk/benefit ratio needs to be considered, given that steroids also may increase risk of infection. Arterial catherisation is best avoided where possible, for fear of aneurysm development at the arterial entry site. People often report that visits to the dentist or oral hygienist result in an outbreak of oral ulcers, which can often be avoided with a short course of steroids prior to the visit.
Pregnancy and Behçet’s syndrome
There is no evidence that people with Behçet’s syndrome have an increased risk of fertility problems, or complications during pregnancy, although women with vascular, neurological or eye involvement need to have a serious discussion with their doctors before proceeding. It is very important to discuss medications with your doctor, as some of the medications that patients are treated with for Behçet’s Syndrome may potentially harm a developing baby if not stopped well in advance of pregnancy.
Prognosis
For the vast majority of people with Behçet’s syndrome, a normal life span is expected. For those with severe eye inflammation, progressive loss of vision was previously a major complication. However, with improving treatments, visual loss now uncommon. Those with purely ‘skin/ulcers/joint’ disease have a very good prognosis.
Key Points
- Behçet’s syndrome is a multisystem condition, the hallmark features being mouth and genital ulcers, although many areas may be affected, including inflammation in the eyes
- Behçet’s syndrome commonly affects the skin, stomach and musculoskeletal systems
- No diagnostic test currently exists for Behçet’s syndrome
- Treatment is based on immunosuppression with agents including steroids, azathioprine, and biologic agents
Acknowledgements
Dr Nicola Ambrose, MB BCh, MRCPI, PhD for producing this web page on Behçet’s syndrome.
Dr Ambrose is a Rheumatologist working at University College London Hospital, having received her training in Behçet’s syndrome working with Prof Dorian Haskard.
Also Vasculitis UK for providing the information.
